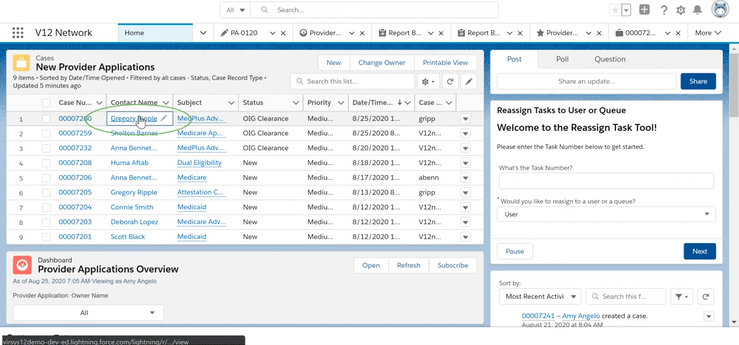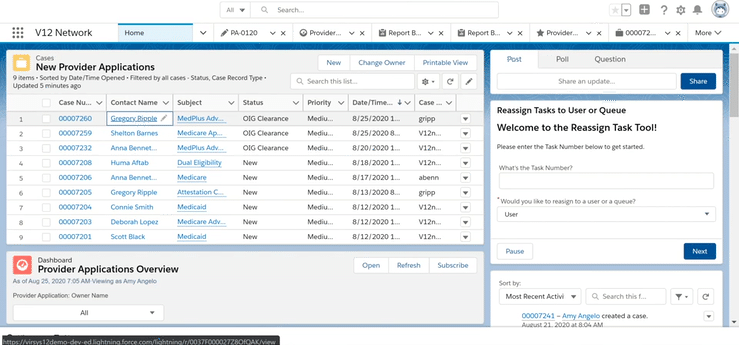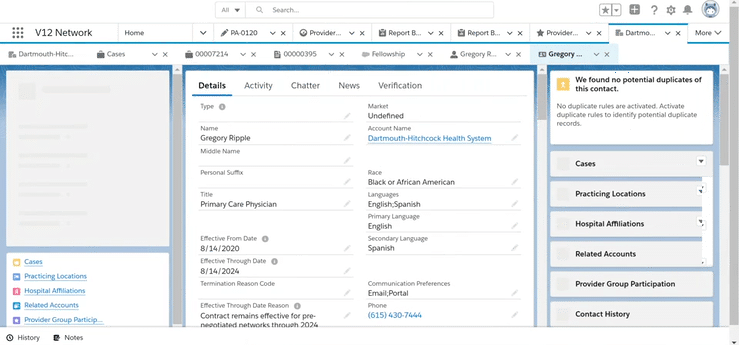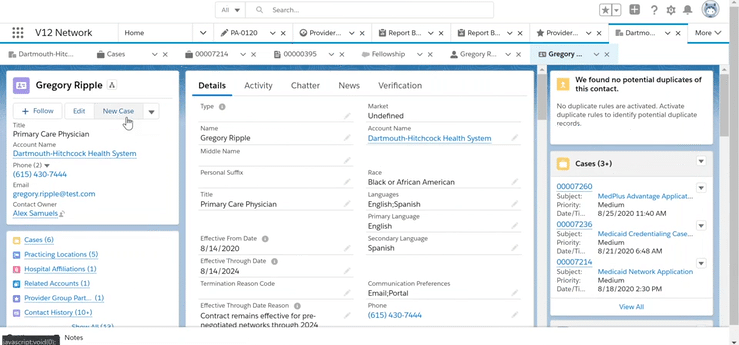
Once you receive the provider information, it has to be validated for accuracy before initiating the credentialing process. What if you could check the practitioners OIG and state exclusions real-time and follow an auditable and structured workflow process to stay on track? You can with the automation in V12 network with API integration to Provider Trust for exclusion checks!
· See an “out of the box” process for reviewing provider application data in V12 Network and Salesforce Health Cloud to verify accuracy before credentialing
· See how integration with Provider Trust makes OIG and exclusion checks easy
· Understand how automation in V12 Network can save thousands of hours of manual work related to processing provider applications for your provider networks